Periodontal disease, or gum disease, is a big concern for dental health as it affects the tissues that hold teeth in place. The way dentists identify and describe the severity of gum disease has recently changed, introducing a system of staging and grading. This approach helps dentists figure out how serious the disease is and how fast it’s progressing. By understanding these AAP stages and grades, patients can get a clearer idea of what their treatment might look like and what they can do to keep their teeth healthy.
If you need periodontal treatment in Utah, we can help! We have two offices located in Salt Lake City and South Jordan. Our experienced staff and periodontists are excited to help you. Click the button below to request an appointment!
Periodontal Staging and Grading
As mentioned above, staging and grading in periodontal disease are tools that dentists use to figure out how severe a patient’s gum disease is and how quickly it might get worse. Staging looks at the current damage caused by the disease, such as how much bone support has been lost around the teeth and whether any teeth have been lost. This helps dentists understand how advanced the disease is and what might be involved in treating it.
Grading, on the other hand, is about predicting how fast the gum disease might progress. It considers things like the patient’s overall health, whether they smoke, and if they have other diseases that could speed up the damage to the gums and bones around the teeth. Grading helps dentists think about how to prevent the disease from getting worse, tailored to each patient’s specific situation.
By using staging and grading together, dentists can get a full picture of a patient’s gum health. This detailed understanding helps them come up with a treatment plan that not only deals with the current problems but also tries to prevent new ones, ensuring they tackle the disease in the most effective way possible.
Stages of Periodontitis
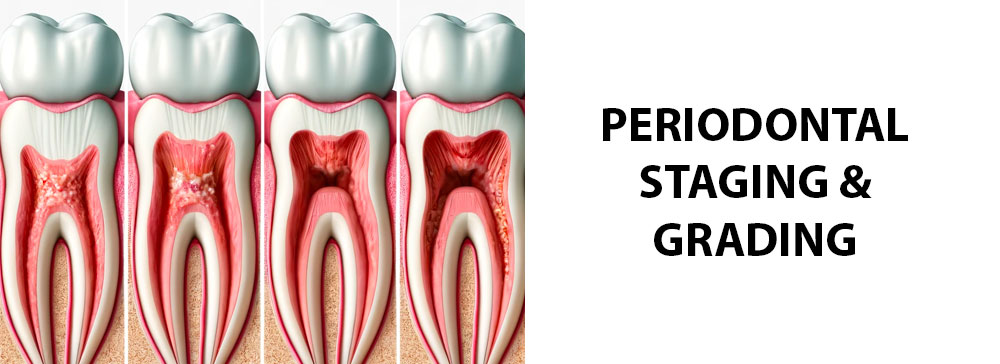
The system is divided into four stages, ranging from least to most severe:
Stage 1: Initial Periodontitis
In the first stage, the damage is relatively mild. Patients might experience some inflammation and bleeding of the gums without significant bone loss. Typically, this stage is associated with slight changes in the depth of the pocket between the tooth and gum, usually up to 4 millimeters deep. Early detection and treatment at this stage can often reverse some of the damage and prevent progression.
Stage 2: Moderate Periodontitis
As the disease progresses to stage 2, there is increased destruction in the supporting bone around the teeth, with pocket depths ranging from 4 to 5 millimeters. Patients may start to notice more bleeding, swelling, and possible receding gums. Bone loss at this stage is evident but has not yet reached critical levels, making timely and effective intervention vital to prevent further deterioration.
Stage 3: Severe Periodontitis with Potential for Tooth Loss
Stage 3 is characterized by significant bone loss (greater than 50%) around the teeth and increased pocket depths beyond 6 millimeters. This stage poses a high risk of tooth loss and may exhibit additional complications such as shifting teeth, minor to moderate furcation involvement (where the disease starts to affect the base of the tooth roots), and possible moderate ridge defects. Treatment at this stage is more complex and aims to manage symptoms and salvage the teeth and bone structure as much as possible.
Stage 4: Advanced Periodontitis with Extensive Tooth Loss and Bone Loss
In the final stage, periodontitis has caused extensive bone loss and deep gum pockets exceeding 7 millimeters. Patients at this stage may suffer from widespread tooth loss, severely receded gums, and complex issues like major furcation involvement and ridge deformities, which significantly impact oral functionality and aesthetics. Management at this stage focuses on controlling the infection and providing solutions for tooth replacement and rehabilitation to restore function and appearance.
Each stage of periodontitis calls for a different level of intervention, from more straightforward cleaning and lifestyle changes in the early stages to potential surgical treatments and restorative procedures in the more advanced stages. Understanding these stages helps patients and dentists make informed decisions about the necessary treatments to manage the disease effectively.
Peri-Implantitis and Peri-Implant Mucositis: What are they?
Peri-implantitis and peri-implant mucositis are conditions that affect the tissues around dental implants, similar to how gum disease affects natural teeth. Both conditions are basically caused by bacterial infections, but they differ in their severity and the tissues they affect.
-
Peri-Implant Mucositis
This condition is akin to gingivitis around natural teeth. It involves inflammation of the mucosal tissues around a dental implant without affecting the bone. Symptoms include redness, swelling, and bleeding on probing around the implant. Peri-implant mucositis is considered reversible with proper oral hygiene and professional cleaning. If treated early, it does not cause lasting damage to the implant or the bone.
-
Peri-Implantitis
Peri-implantitis is the more severe condition and is comparable to periodontitis in natural teeth. It involves inflammation that affects not only the soft tissues but also leads to bone loss around the implant. Symptoms include the signs seen in peri-implant mucositis, along with the loss of supporting bone, which can be detected through radiographs or during a clinical examination. Peri-implantitis can lead to implant failure if not addressed quickly.
Necrotizing Periodontal Diseases
Necrotizing periodontal diseases are a severe form of periodontal conditions that are characterized by the death of gum tissue, periodontal ligaments, and supporting bone. These diseases are marked by rapid tissue destruction and can lead to significant oral and systemic complications if not treated promptly.
- Necrotizing Ulcerative Gingivitis (NUG): This is the initial stage of necrotizing periodontal diseases, primarily affecting the gum tissue. It’s often characterized by painful ulcers, bleeding, and a noticeable foul odor. Patients might experience extreme pain and bleeding even with gentle brushing. Other symptoms include a metallic taste in the mouth and excessive salivation.
- Necrotizing Ulcerative Periodontitis (NUP): When the condition progresses from NUG, it can evolve into NUP, where the infection spreads from the gums to deeper periodontal structures, including the bone. This stage involves more severe destruction, including loss of attachment and bone, which can lead to tooth mobility and loss if untreated.
The hallmark features of necrotizing periodontal diseases are rapid onset and tissue necrosis, which are visibly noticeable as grayish sloughing areas of dead tissue. These conditions are more common in individuals with systemic conditions such as immunodeficiency, malnutrition, and stress, and are also associated with smoking.
Treatment involves immediate professional care, which might include the removal of necrotic tissue, administration of antibiotics, and rigorous oral hygiene. Additionally, addressing underlying systemic conditions or lifestyle factors such as smoking and stress management is crucial for effective management and prevention of recurrence.
What Causes Periodontitis
Here’s a breakdown of its causes and what it can be a symptom of:
- Plaque Accumulation: The primary cause of periodontitis is the accumulation of plaque, a sticky film composed mainly of bacteria. If plaque isn’t removed through regular brushing and flossing, it can harden into tartar, causing more gum inflammation.
- Poor Oral Hygiene: Inadequate brushing and flossing make it easier for plaque to build up along the gumline, creating an environment where periodontitis can develop.
- Tobacco Use: Smoking or chewing tobacco is known to contribute significantly to the onset and progression of periodontal disease.
- Genetics: Some individuals are more susceptible to periodontal disease genetically, which can accelerate the progression despite having good oral hygiene habits.
- Medications: Certain medications can cause dry mouth, reducing saliva production, which helps protect the teeth and gums. Some drugs can also cause abnormal growth of gum tissue, making it difficult to keep the teeth and gums clean.
- Chronic Conditions: Conditions like diabetes, rheumatoid arthritis, and other immune-related illnesses can interfere with the body’s ability to regulate inflammation, which may worsen the condition of the gums.
What Periodontitis is a Symptom Of
Periodontitis itself is typically more of a result than a symptom, but it can be indicative of several broader health issues:
-Underlying Systemic Diseases: Because periodontitis can be linked to inflammation, it might indicate the presence of systemic diseases such as diabetes, heart disease, or rheumatoid arthritis.
-Immune System Disorders: Individuals with compromised immune systems, such as those with HIV/AIDS or those undergoing cancer treatments, are more susceptible to severe periodontitis.
-Nutritional Deficiencies: Poor nutrition can weaken the immune system and decrease the body’s ability to fight infection, including gum infections. Deficiencies in vitamins C and K have been linked to gum health.
We recommend scheduling regular dental check-ups as they are very important when it comes to diagnosing and managing periodontitis.
The Periodontal Staging and Grading Guide Conclusion
Periodontitis is a severe gum disease primarily caused by the buildup of plaque, influenced by factors such as poor oral hygiene, tobacco use, genetics, certain medications, and systemic health conditions. This condition not only affects oral health but may also signal broader systemic issues.
At Utah Periodontal Specialists, we know how important your gum health is. That’s why we’ve made it easy to get the care you need with our offices in Salt Lake City and South Jordan. Call or go online to schedule your check-up or treatment—it’s all about keeping you healthy. Count on us for all your periodontal needs!


Recent Comments