DIAGNOSIS
Diagnosing Periodontal Disease
Periodontal disease is diagnosed by your dentist or dental hygienist during a periodontal examination. This type of exam should always be part of your regular dental care at least twice a year.
Diagnosing periodontal disease, a common but serious gum condition, involves a comprehensive dental examination. Dentists use a special tool called a periodontal probe to measure the depth of the spaces between the gums and teeth, known as periodontal pockets. Healthy gums typically have shallow pockets, but deeper pockets may indicate periodontal disease.
Periodontal Disease in South Jordan and Salt Lake City
Our offices in South Jordan and Salt Lake City emphasize the importance of regular check-ups, professional cleanings, and patient education to combat periodontal disease. We offer a range of services, from routine preventive care to advanced treatments for more severe cases. Early detection and intervention are key in managing and preventing the progression of periodontal disease.
Gum Disease in South Jordan and Salt Lake City
Gum disease and periodontal disease are terms often used interchangeably, but they describe different stages of the same oral health condition affecting the gums and bones around the teeth. The progression can be broken down into two main stages:
1. Gingivitis:
This is the initial stage of gum disease. It is characterized by inflammation of the gums, usually caused by the build-up of plaque, a sticky film of bacteria that forms on teeth. Symptoms of gingivitis include red, swollen, and bleeding gums, especially during brushing or flossing. Gingivitis is reversible with good oral hygiene and professional dental care.
2. Periodontitis:
If gingivitis is left untreated, it can advance to periodontitis, a more severe form of gum disease. In periodontitis, the inner layer of the gum and bone pull away from the teeth and form pockets, which can become infected. This stage can lead to more significant issues, including the destruction of the supporting bone and connective tissue that holds teeth in place. Periodontitis can result in tooth loss and requires more complex treatment.
How to Prevent Periodontal and Gum Disease
Preventing periodontal disease involves maintaining good oral hygiene and regular dental care. Key practices include:
- Brushing Teeth Regularly: Brush at least twice a day using fluoride toothpaste. This helps remove dental plaque, a key factor in periodontal disease.
- Flossing Daily: Flossing removes food particles and plaque from between the teeth and under the gum line, areas where a toothbrush can’t always reach.
- Regular Dental Check-ups: Visiting a dentist or dental hygienist regularly for cleanings and examinations is crucial. They can remove hardened plaque (tartar) and identify early signs of gum disease.
- Healthy Diet: Eating a balanced diet and limiting sugary snacks can contribute to better oral health.
- Avoiding Tobacco: Smoking or chewing tobacco significantly increases the risk of periodontal disease and can hinder the healing process of the gums.
- Using Mouthwash: Therapeutic mouthwashes can help reduce plaque and remove food particles.
How We Can Help
At Utah Periodontal Specialists, we are committed to providing expert care for those experiencing signs or symptoms of periodontal disease. Our experienced team utilizes the latest techniques and technology to diagnose and treat various stages of gum disease effectively. Whether you’re noticing early signs like gum sensitivity, redness, or bleeding, or dealing with more advanced symptoms such as receding gums or tooth looseness, our specialists are equipped to offer personalized treatment plans.
We focus on minimally invasive procedures to ensure patient comfort and quicker recovery times. Our goal is to not only treat the existing condition but also to educate our patients on maintaining optimal oral health to prevent future occurrences of periodontal disease. Trust us to be your partners in achieving and maintaining a healthy, beautiful smile.
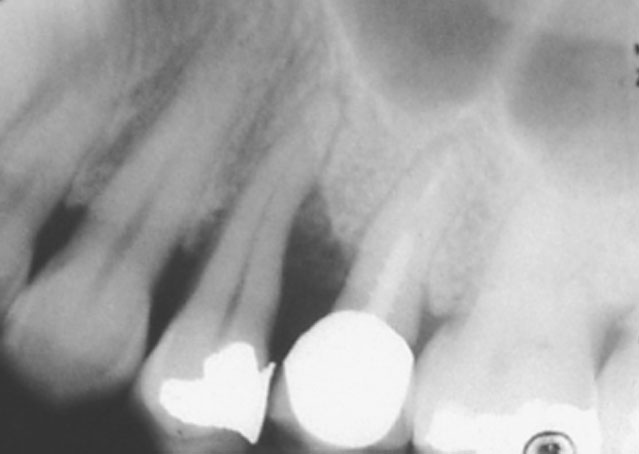
X-Rays
X-rays are used to diagnose bone loss surrounding the roots of the teeth. If evidence of bone loss is seen on x-rays periodontal treatment is mandatory. If left untreated the likelihood of tooth-loss is high.
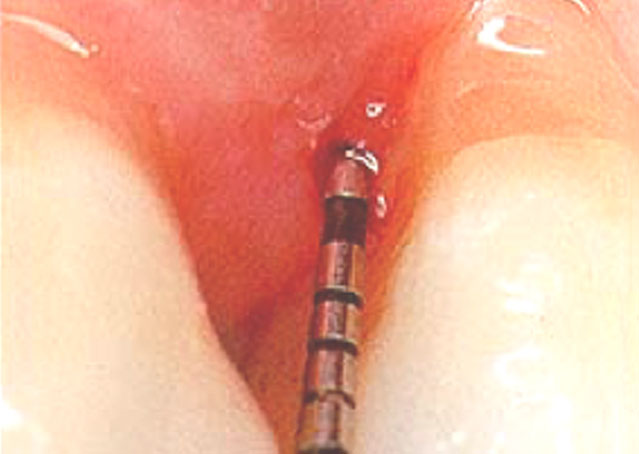
Periodontal Probe
A periodontal probe (small dental instrument) is gently used to measure the sulcus (pocket) between the tooth and the gums. The depth of a healthy sulcus measures three millimeters or less and does not bleed. The periodontal probe helps indicate if pockets are deeper than three millimeters. As periodontal disease progresses, the pockets usually get deeper. Your dentist or hygienist will use pocket depths, amount of bleeding, and tooth mobility to make a diagnosis that will fall into a category below:
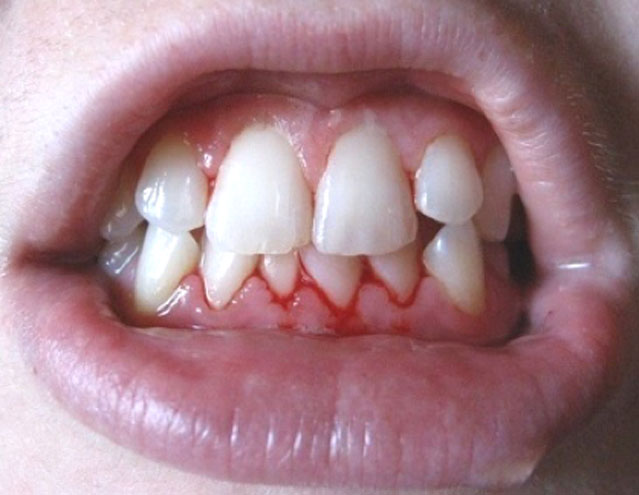
Gingivitis
Gingivitis is the first stage of periodontal disease. Plaque and its toxin by-products irritate the gums, making them tender, inflamed, and likely to bleed.
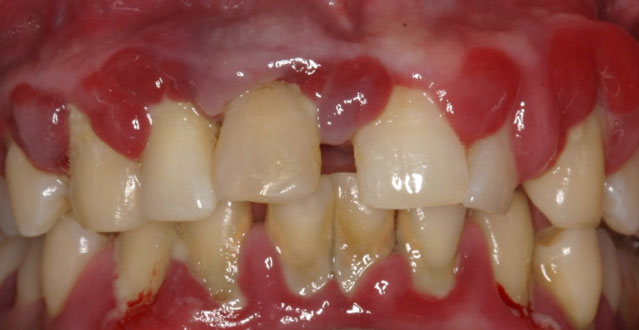
Mild to Moderate Periodontal Disease
Plaque hardens into calculus (tartar). As calculus and plaque continue to build up below the gum line, the gums begin to recede from the teeth. Deeper pockets form between the gums and teeth and become filled with bacteria and pus. The gums become very irritated, inflamed, and bleed easily. Slight to moderate bone loss may be present.
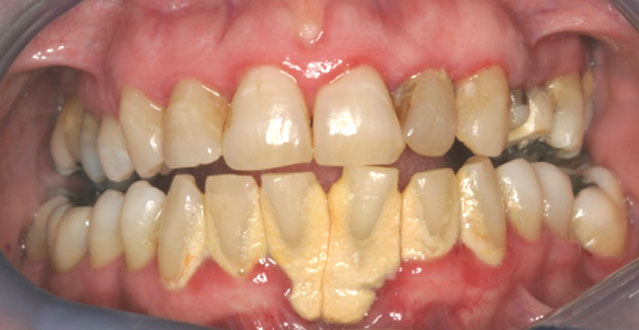
Severe Periodontal Disease
The teeth lose more support as the gums, bone, and periodontal ligament continue to be destroyed by tartar and bacteria. Unless treated, the affected teeth will become very loose and may be lost.
PREVENTION
LEARN MORE

Treatment
Scaling, root planing and bite adjustment can improve the health of tissue, often being curative themselves.

Prevention
Daily brushing and flossing removes plaque from teeth and gums and helps reduce tartar deposits.

Periodontal Disease
Periodontal disease affects more than 80% of Americans by the age of 45. Certain factors contribute to its progression.

